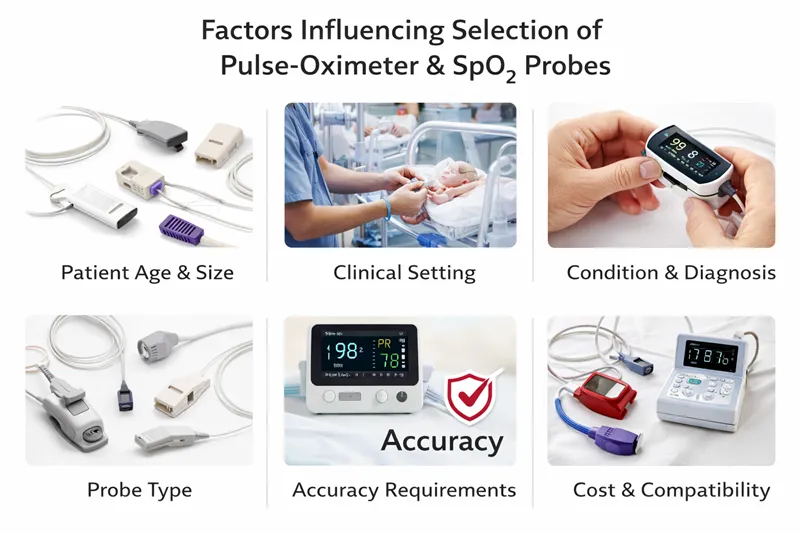
With multiple technologies, brands, probe types, and
measurement methods available, choosing the right pulse oximeter and SpO₂ probe
can be confusing. Questions often arise: Is finger transmission better than
forehead reflectance? Should one choose Masimo SET or Nellcor OxiMax? Is a
standalone oximeter better than an integrated monitor?
This blog explores the key factors influencing the selection
of pulse oximeters and SpO₂ probes, helping clinicians, biomedical engineers,
and hospital administrators make informed decisions.
What Is Pulse Oximetry?
Pulse oximetry is a non-invasive technique used to measure
the percentage of oxygen-saturated hemoglobin in the blood (SpO₂). It works by
passing light through or reflecting light off vascular tissue and analyzing how
much light is absorbed by oxygenated versus deoxygenated blood.
Because oxygen saturation is a critical marker of
respiratory function, pulse oximeters are indispensable in:
- Critical
care units
- Anesthesia
and surgery
- Neonatal
and pediatric care
- Emergency
and trauma care
- Post-operative
recovery
Why Choosing the Right Pulse Oximeter Matters
An inaccurate or unreliable pulse oximeter can lead to:
- Missed
hypoxemia
- Delayed
clinical intervention
- False
alarms and alarm fatigue
- Poor
patient outcomes
Therefore, selecting the right device is not about brand
preference alone it is about clinical accuracy, patient safety, and usability.
Key Factors Influencing the Selection of Pulse Oximeters
1. Accuracy and Performance in Challenging Conditions
One of the most important considerations is how well the
device performs under real-world clinical conditions such as:
- Patient
movement
- Low
perfusion states
- Poor
signal quality
- Ambient
light interference
Advanced technologies like Masimo SET and Nellcor OxiMax are
designed to improve accuracy during motion and low perfusion, making them
suitable for ICUs and critical care settings.
2. Measurement Technology: Transmission vs Reflectance
Transmission Pulse Oximetry
- Commonly
used in finger, toe, or ear probes
- Light
passes through tissue
- Widely
used in adults and cooperative patients
Pros:
- Proven
accuracy
- Cost-effective
- Simple
to use
Cons:
- Less
reliable in poor perfusion or excessive movement
Reflectance Pulse Oximetry
- Used
in forehead or wrist sensors
- Light
reflects off tissue instead of passing through
Pros:
- Better
performance in low perfusion states
- Useful
during shock or vasoconstriction
Cons:
- Higher
cost
- Limited
availability of probes
The choice depends on patient condition and clinical
environment.
3. Type of Clinical Application
Different care areas have different requirements:
- ICU
& OT: High accuracy, motion tolerance, integration with monitors
- Recovery
Room: Fast response and reliable trend monitoring
- General
Wards: Portable, easy-to-use standalone devices
- Neonatal
Care: Special probes with gentle adhesion and high sensitivity
Matching the oximeter to the clinical use case is essential.
4. Standalone vs Integrated Pulse Oximeters
Standalone Pulse Oximeters
- Portable
and compact
- Ideal
for wards, transport, and spot checks
Integrated SpO₂ Modules
- Built
into multiparameter monitors
- Central
monitoring and data recording
- Preferred
in ICUs and OTs
Hospitals often use a combination of both depending on
workflow needs.
5. Selection of SpO₂ Probes
The probe plays a critical role in measurement accuracy.
Common Types of SpO₂ Probes
- Adult
finger probes
- paediatric
probes
- Neonatal
wrap probes
- Ear
probes
- Forehead
probes
Reusable vs Disposable Probes
Reusable Probes:
- Cost-effective
long-term
- Require
proper cleaning and maintenance
Disposable Probes:
- Reduced
infection risk
- Ideal
for isolation and critical care
6. Patient Factors
Patient characteristics significantly influence probe
selection:
- Age
(adult, paediatric, neonatal)
- Skin
thickness and pigmentation
- Perfusion
status
- Presence
of edema or injury
For neonates and infants, using size-appropriate probes is
non-negotiable.
7. Motion Tolerance
Patients in ICUs, emergency departments, or paediatrics
often move. Technologies that reduce motion artifacts help avoid false alarms
and improve clinical confidence.
This is where motion-tolerant algorithms play a major role.
8. Compatibility and Brand Considerations
Not all probes are interchangeable. Compatibility with
existing monitors is crucial. Popular technologies include:
- Masimo
SET
- Nellcor
OxiMax
Hospitals often standardize brands to simplify training,
maintenance, and inventory management.
9. Ease of Use and Ergonomics
Devices should be:
- Simple
to operate
- Easy
to clean
- Comfortable
for patients
- Durable
for frequent use
Good design improves compliance and efficiency.
10. Cost, Maintenance, and Service Support
Initial cost is only one part of the equation. Consider:
- Cost
of probes and consumables
- Calibration
requirements
- Availability
of service support
- Warranty
and lifecycle costs
Platforms like Aarogyaa Bharat help healthcare providers
compare and source quality pulse oximeters and compatible SpO₂ probes from
trusted manufacturers.
Common Mistakes to Avoid
- Choosing
based on brand popularity alone
- Ignoring
probe compatibility
- Using
adult probes on pediatric patients
- Neglecting
maintenance and calibration
Frequently Asked Questions (FAQs)
Q1. Is forehead pulse oximetry more accurate than finger
probes?
Forehead probes may perform better in low perfusion states, but finger probes
are accurate in most routine cases.
Q2. Can one probe be used for all patients?
No, probe selection must match patient size and condition.
Q3. How often should SpO₂ probes be replaced?
Based on manufacturer guidelines and wear-and-tear.
Q4. Are integrated monitors better than standalone
oximeters?
Each serves different clinical needs; both are essential in hospitals.
Conclusion
Selecting the right pulse oximeter and SpO₂ probe is a
balance between technology, clinical need, patient safety, and
cost-effectiveness. There is no single “best” pulse oximeter for all situations
only the right choice for the right application. By understanding the factors
that influence selection, healthcare providers can ensure accurate monitoring,
timely interventions, and better patient outcomes.
In modern healthcare, a reliable pulse oximeter is not just
a device it is a silent guardian of patient safety.